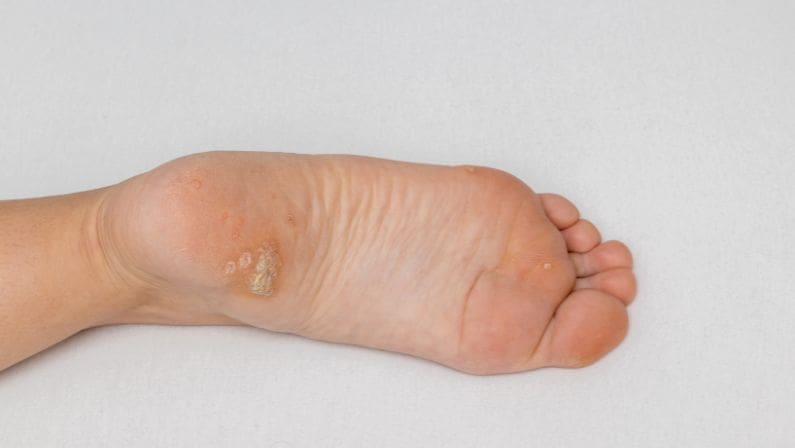
Plantar heel pain (commonly referred to as “plantar fasciitis”) is defined as pain or discomfort in the bottom of the heel. It is generally characterised in its early stages by pain or discomfort when rising from rest, especially if a lot of time has been spent on the heel during the day. In the case of morning pain, it will generally occur if a big day was had the day before.
In its infancy this discomfort seems to settle after a couple of minutes of walking around, however if the problem is left to worsen it can get to a stage where any type of weight bearing activity is painful. I have seen cases where patients have had to resort to the use of crutches and moonboots just to perform basic daily tasks.
Plantar Heel Pain can be caused by many different risk factors. The main factors I see are a sudden change in activities (i.e. increased walking, running, jumping, employment that requires more standing), and changes in footwear. Some people are predisposed because of biomechanics (e.g. poor foot function or poor proximal hip stability) or systemic factors (e.g. age, menopause, elevated cholesterol, increased susceptibility to pain, weight etc). Predisposed people may develop Plantar Heel Pain with even subtle changes in their activity.
When treating the condition my primary aims are to address two main issues. The first is to reduce compressive load (squashing up against the bottom of the calcaneus or heel bone) and the second is to reduce shear forces around the heel generally increased by foot function or footwear.
I feel it is important to address Plantar Heel Pain as soon as possible and to be aggressive with treatment. Generally speaking, the longer a patient has had this problem the longer it will take to resolve it.
My general treatment plan for Plantar Heel Pain is as follows:
- Taping in the first instance. In particular to support the fat pad under the heel so it can act as a “cushion” and reduce the compressive load on the heel.
- Footwear change. This does depend on the foot type we are treating, however the main aims are to reduce the compressive and shear forces on the heel.
- Strengthening Program for the small muscles of the foot
- Calf Muscle Stretching
- Manual Therapy to increase the ankle’s range of motion
- Dry Needling of the intrinsic muscles to treat painful trigger points
- Orthoses. We now have evidence that custom foot orthoses provide for much better outcome at 12 weeks than exercises and footwear changes alone and in my experience can resolve 95% of these cases.
If these interventions fail (which may be the case if the problem is long standing) other interventions include:
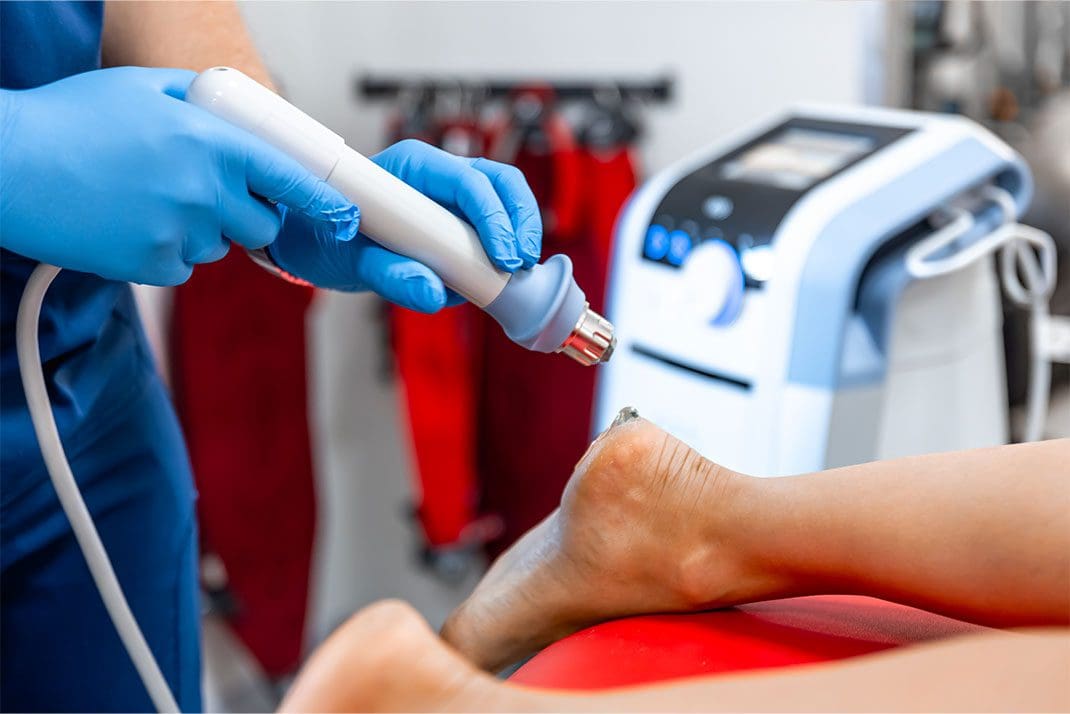
- Extracorporeal Shockwave Therapy
- Corticosteroid Injections
- Surgery such as a plantar fasciotomy
Plantar Heel Pain is a health issue that left without treatment can become debilitating. My advice is if you are suffering with this or something similar, please don’t hesitate in seeking assistance. The sooner it is addressed the sooner you can get back to doing what you love doing, pain free.